A pituitary adenoma is generally a benign, slow growing tumor that occurs in the pituitary gland. The pituitary gland is a small, bean shaped structure that lies at the base of the brain. It has a central role in the regulation of hormones that affect the body such as Adrenocorticotropic hormone (ACTH), Growth hormone (GH), Prolactin, and Thyroid-stimulating hormone (TSH).
Approximately 1 in 1,000 individuals have pituitary adenomas. They are generally not cancerous but may invade nearby structures. They are classified based on size. A microadenoma is less than 1 cm in diameter whereas a macroadenoma is larger than 1 cm in size.
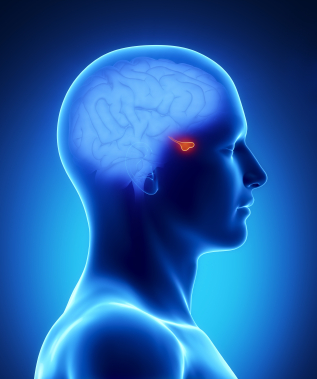
Based on whether the pituitary adenoma is a hormone-producing or hormone-inactive tumor, the patient will present with different symptoms. Hormone-producing tumors will make excessive amounts of an active hormone so symptoms present as a hormonal imbalance. The three most common hormone-producing adenomas are Prolactinomas, Growth hormone-secreting pituitary adenoma, and ACTH-secreting pituitary adenoma.
If the patient has a large hormone-inactive or hormone-producing tumor, it may compress surrounding brain structures due to its size. Large pituitary tumors may compress the pituitary gland contributing to pituitary failure, which can lead to sexual dysfunction, inadequate body cortisol levels, and hypothyroidism. Other possible presentations relating to compression of brain structures include visual loss, headache, the “stalk effect”, and pituitary apoplexy. The “stalk effect” is due to the compression of the pituitary stalk, the structure connecting the brain to the pituitary gland, which leads to a mild elevation in the hormone prolactin. Higher levels of prolactin in females can contribute to irregular menstrual cycles. Pituitary apoplexy presents with an abrupt headache and visual loss. It can occur under two different situations. The pituitary adenoma can bleed internally causing a sudden increase in size or the tumor can outgrow its blood supply and the dead tissue will swell.
Pituitary adenomas can be diagnosed based on endocrine function testing, imaging, and visual field testing. Often times, visual problems may be the only symptom present. Optometrists and ophthalmologists should seriously consider the possibility of a pituitary tumor when the patient presents with an unexplained loss of visual field (especially peripheral vision), double vision, or blurred vision as the growth of a pituitary tumor can cause compression on the visual pathway (retina, optic nerve, etc). A delay in diagnosis of a pituitary adenoma may result in permanent loss of vision due to the damage caused by this compression. Endocrine function testing evaluates cortisol, follicle-stimulating hormone, lutenizing hormone, insulin growth factor-1, prolactin, testosterone/estradiol, and thyroid hormone levels. The preferred method of imaging is MRI, which screens for adenomas larger than 4 mm.
Treatment for pituitary adenomas depends on the presence of hormone production, size of the tumor, invasion of the tumor into surrounding structures, and the age and health of the patient. Drug therapy is used to treat hormone-producing tumors. For example, bromocriptine and cabergoline are used to treat tumors secreting prolactin because these medications decrease prolactin levels and tumor size. Pituitary adenomas that require surgery are usually minimally invasive techniques, where the tumor is removed through the nose. On the other hand, radiation therapy involves high doses of radiation being delivered to the tumor. It is a treatment utilized for pituitary adenomas that cannot be controlled by drug therapy or surgical intervention. Patients have the best outlook when the entire tumor can be removed.